Some shoulders can be saved with surgery that repairs a rotator cuff or removes a bone spur. But when a shoulder cannot be saved, shoulder replacement surgery may be the answer. It has been steadily refined to provide individuals with functioning shoulders and predictable improvement in pain and is the fastest-growing joint replacement surgery performed today.
 David Peterson (pictured at right) remembers the exact moment he knew his left shoulder was seriously damaged. Despite living with chronic pain, the Acton resident, 64, continued to work as a carpenter — gripping tools, climbing ladders and lifting a 70-pound tool bag.
David Peterson (pictured at right) remembers the exact moment he knew his left shoulder was seriously damaged. Despite living with chronic pain, the Acton resident, 64, continued to work as a carpenter — gripping tools, climbing ladders and lifting a 70-pound tool bag.
“The pain slowly snuck up on me and became the ‘normal,’” recalls Mr. Peterson. “Despite the pain, I never missed work. I kept moving and tried to take on lighter duties. After a while, it didn’t register.”
But one day, it did. “I was driving my van, and just turning the wheel caused sudden pain. That was definitely the moment.” He made an appointment to see his primary care physician, Sandeep Jain, MD, who administered a cortisone shot and prescribed physical therapy. About a month later, Mr. Peterson had an appointment to see Paul Re, MD, an Emerson orthopedic surgeon who specializes in shoulder surgery.
“It’s not uncommon for patients to describe how a simple thing — like turning the wheel of his van — causes pain that has them seeking medical care,” says Dr. Re. “Over time, you can wear out the cartilage in a joint and, with a simple action, reach a threshold. A piece of cartilage can tear away from the bone, leaving it exposed to bruising.”
Dr. Re examined Mr. Peterson’s shoulder and was straightforward. “He said I needed a shoulder replacement, and it would take the pain away,” says Mr. Peterson. “I said ‘you’re on.’ I knew I had to have the surgery, but I needed to buy some time so I could complete the job I was on.”
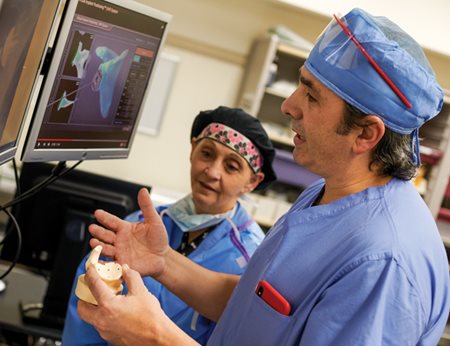 Ultrasound-guided cortisone injections did the trick. “Patients often ask what we can do to delay surgery,” notes Dr. Re (pictured at left with Karen Robinson, RN). “Others either cannot have surgery or don’t want to have surgery. We can keep some people going for a while with cortisone injections or by performing minimally-invasive surgery that loosens up the shoulder ligament.”
Ultrasound-guided cortisone injections did the trick. “Patients often ask what we can do to delay surgery,” notes Dr. Re (pictured at left with Karen Robinson, RN). “Others either cannot have surgery or don’t want to have surgery. We can keep some people going for a while with cortisone injections or by performing minimally-invasive surgery that loosens up the shoulder ligament.”
Mr. Peterson’s surgery was scheduled for May 2018. He wasn’t surprised when Dr. Re told him that his right shoulder was also in serious shape. It would be replaced once Mr. Peterson recovered from the first surgery.
Two surgeries and minimal pain
After enduring pain that affected his waking hours and disrupted his sleep, Mr. Peterson woke up after the surgery with no pain in his left shoulder. “I felt a little discomfort, but I didn’t need pain medication — not even Tylenol,” he says. “I just applied ice throughout my rehab.”
Dr. Re isn’t surprised when individuals report that they have minimal pain after shoulder replacement surgery. “We address pain with regional anesthesia before the surgery is performed,” he explains, “but in these patients, we replace painful surfaces with smooth ones — new shoulder components. We’re not operating on raw, irritated tendons, so they experience a great deal of relief after surgery. That is partly to do with how long they’ve been in pain.”
Mr. Peterson stayed one night at Emerson and headed home to begin his rehab. “It went great,” he says. “I kept the shoulder immobilized, as Dr. Re instructed, and then returned to the physical therapist who had stretched the shoulder prior to my surgery.
She told me the range of motion was much better in the right shoulder. That was encouraging as I headed back to Emerson for my second shoulder replacement.”
The second surgery, performed in December 2018, was even easier. “There’s no pain at all now,” says Mr. Peterson, who plans to return to work in June but understands he will have some limitations. Like his father and grandfather — also carpenters — Mr. Peterson has clients who depend on him and are eager to see him back on the job. “I know I have to be careful not to overdo it.”
“Shoulder replacement surgery is being performed more often because improved shoulder components and the refined surgical technique have made the surgery more successful, and also because of the aging population,” notes Dr. Re. “Many of these individuals are in their 70s or older, and they want to stay in their homes, so they need to be able to drive and cook.” Approximately 10 percent of Dr. Re’s patients have both shoulders replaced.
In about half of cases, the shoulder lacks a healthy rotator cuff, and he performs reverse shoulder replacement surgery, which reverses the location of the shoulder components. Dr. Re is one of very few surgeons outside of Boston using a CT-guided implant positioning system to plan patient-specific surgery.
Long before anyone attempted to perform hip or knee replacement surgery, the focus was on shoulder replacement — a way to keep the body’s most complicated joint working. Today, the shoulder is the fastest-growing joint replacement surgery.
“They are among my happiest patients,” says Dr. Re, “because they’re out of pain, and they’ve regained function.”

