According to the non-profit organization Beyond Type 1, approximately 1.45 million Americans are living with Type 1 Diabetes, and the rate of people diagnosed annually is growing. Bridget, Emerson's Internal Communications Manager, shares the story of her son's diagnosis to bring attention to the signs you can watch for in your own loved ones and how, through the support of incredible technology, skilled medical providers, and a lot of love, Type 1 Diabetes does not have to get in the way of a happy and healthy life.

November 5, 2018, was the day our lives changed forever. But let me back up a bit – in October of that year, my motherly instincts sensed something medically was up with my oldest son, Hunter. Most notably, he was extremely thirsty, regardless of how much he had to drink. Peculiar but not yet alarming, I made a mental note of it and went about our lives. I also noted that he had to urinate more often, but he had been drinking so much, so naturally, he had to pee!
Over the next month or so, his symptoms continued progressing, and he began visibly losing weight. I find it challenging to look at photos from that time, as he so obviously looked sick. They say hindsight is 20/20, which is entirely accurate in this case. A mix of seeing him every day and a good dose of denial would not allow me to fully see the direness of the situation when I was in it. But ultimately, motherly instinct won over and would no longer let me deny it.
We saw Hunter's pediatrician nearly immediately, as his list of symptoms likely set off some alarm bells for them. There, they pricked his finger – his blood sugar was 482 – a number I will never forget. For reference, a "normal" blood sugar is around 80 – 120, so 482 was off the charts. They also confirmed sugar in his urine – a telltale sign of what I already knew.
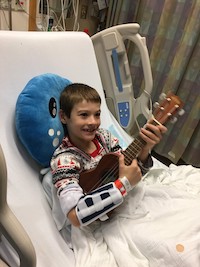 Hunter's kind, incredible pediatrician delivered the unfortunate diagnosis of Type 1 Diabetes with such compassion. He told us we needed to go home and pack our bags for a few nights' stay at Children's Hospital in Boston and that the Emergency Department there would be expecting us as soon as possible. I wanted to cry and scream, but I also knew that Hunter had no idea what was going on, and I didn't want to scare him, so I held it together. I calmly told Hunter about his diagnosis and what it meant for the immediate future. At eight years old, he could not possibly grasp the gravity of the situation and looked forward to a few days off from school.
Hunter's kind, incredible pediatrician delivered the unfortunate diagnosis of Type 1 Diabetes with such compassion. He told us we needed to go home and pack our bags for a few nights' stay at Children's Hospital in Boston and that the Emergency Department there would be expecting us as soon as possible. I wanted to cry and scream, but I also knew that Hunter had no idea what was going on, and I didn't want to scare him, so I held it together. I calmly told Hunter about his diagnosis and what it meant for the immediate future. At eight years old, he could not possibly grasp the gravity of the situation and looked forward to a few days off from school.
I drove through the haze of my tears, calling family members to tell them the news. During our stay at Children's, we received a crash course in caring for Hunter. We would be sent home to practice what we were taught in just a few days, knowing that the stakes were life or death. Every meal involved a complex math equation where too much or too little insulin, delivered at the wrong time, could have dangerous consequences.
 We recently celebrated Hunter's fifth "diaversary," as it's called. Why commemorate the diagnosis of a life-altering disease, you ask? Well, because that is the day Hunter's life was saved. That day, he was given a chance to go on living like every other kid. We celebrate the fact that we were fortunate, as not everybody recovers. Symptoms of Type 1 are often overlooked as a virus or other childhood illness. Some children are rushed to the hospital in critical condition, suffering from diabetic ketoacidosis, because their blood sugar was too high for too long. Their body shuts down from trying to rid itself of the excess sugar, and for some, tragically, it is even fatal.
We recently celebrated Hunter's fifth "diaversary," as it's called. Why commemorate the diagnosis of a life-altering disease, you ask? Well, because that is the day Hunter's life was saved. That day, he was given a chance to go on living like every other kid. We celebrate the fact that we were fortunate, as not everybody recovers. Symptoms of Type 1 are often overlooked as a virus or other childhood illness. Some children are rushed to the hospital in critical condition, suffering from diabetic ketoacidosis, because their blood sugar was too high for too long. Their body shuts down from trying to rid itself of the excess sugar, and for some, tragically, it is even fatal.
This is why I share my story today. Know the signs to look for in your children so you can treat them fast and get the help and support you need. The most common symptoms include:
- Excessive thirst
- Frequent Urination/bed-wetting
- Dry Mouth
- Fatigue and weakness
- Increased appetite
- Unexplained weight loss
- Slow healing cuts
The truth is Hunter still has good days and bad days when it comes to his diabetes. Five years out, though, most days are good. Initially, giving insulin with every meal seems daunting and impossible. Today, it has become just part of our lives. Today's diabetes technology is incredible, providing more information through continuous glucose monitoring (CGM) and automatic up-to-the-minute insulin delivery adjustments through a pump that "speaks" to his CGM - essentially an artificial pancreas! A cure is next, and I hope more than anything I get to see the look on his face when that day comes.
 Hunter makes me proud every single day. He is primarily independent in his disease management and never lets it stop him. He loves to play football, is a great wrestler, and is the kindest, most thoughtful, and incredible kid I know (don't tell my other two boys!).
Hunter makes me proud every single day. He is primarily independent in his disease management and never lets it stop him. He loves to play football, is a great wrestler, and is the kindest, most thoughtful, and incredible kid I know (don't tell my other two boys!).
Some facts about Type 1 Diabetes:
- It is an auto-immune disease – it is unknown what triggers it, but genetics can sometimes play a part, as can environmental factors such as a virus.
- The auto-immunity triggers an attack on the insulin-producing cells of the pancreas.
- Insulin's function is to take the glucose (from our food and our body’s own stored glucose) and deliver it to our body's cells to give us energy.
- When a Type 1 diabetic does not receive insulin, glucose will remain in the blood, causing high blood sugar.
- High blood sugar will cause increased thirst and urination as the body works to flush the excess glucose.
- When the body's cells do not receive energy from glucose, they use stored fat for energy instead. This results in drastic and sudden weight loss.
- There are numerous factors that can impact blood sugar, for example exercise, hormonal fluctuations, time of day, etc. Keeping blood sugar in range is both a science and an art.
- Before the discovery of insulin in 1921, a diagnosis of Type 1 Diabetes was fatal.
- There is neither a cure nor lifestyle changes that will treat Type 1 Diabetes. The only treatment is insulin.
This is my personal story as someone who is not a healthcare provider. The opinions expressed in this article are not those of Emerson Health.
If you or someone you love are experiencing symptoms, contact your primary care provider or visit emersonhospital.org/findadoc.

