The number of surgical specialties offered at Emerson continues to grow. This article highlights four areas where our patients are benefiting from advanced procedures, as well as the experience and insights of our physicians.
New procedure for chronic plantar fasciitis
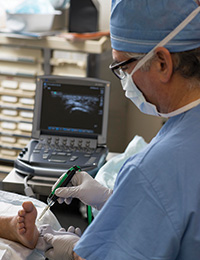 Gregory Catalano, DPM, (pictured at right) an Emerson podiatrist, offers patients a range of treatments for plantar fasciitis. He is one of just a few Massachusetts podiatrists providing a new procedure, ultrasonic percutaneous fasciotomy, to those with the chronic form, plantar fasciosis, characterized by degenerative changes.
Gregory Catalano, DPM, (pictured at right) an Emerson podiatrist, offers patients a range of treatments for plantar fasciitis. He is one of just a few Massachusetts podiatrists providing a new procedure, ultrasonic percutaneous fasciotomy, to those with the chronic form, plantar fasciosis, characterized by degenerative changes.
“This procedure uses ultrasound energy to debride damaged tissue,” Dr. Catalano explains, noting that a quarter-inch incision is large enough for him to introduce the probe. “I like this technology because we’re not cutting the fascia, so its structural integrity is left intact. Also, using ultrasound allows us to visualize what we’re doing.”
Some patients also receive an injection of growth factors to promote healing. Although it does not require general anesthesia, and recovery is much quicker than the traditional surgery, which requires a much larger incision, ultrasonic percutaneous fasciotomy does require recovery time of six to eight weeks.
“As I tell patients, it’s not as though the pain will disappear,” says Dr. Catalano. “They typically need to use a walking boot for a couple of weeks, and it takes a few months for the foot to heal completely.”
Laparoscopic hysterectomy
Consensus statements by two major professional groups have endorsed laparoscopic over traditional abdominal hysterectomy. However, today more than 50 percent of hysterectomies performed in the U.S. for benign diseases — abnormal uterine bleeding, fibroids, endometriosis and pelvic organ prolapse — are open procedures.
Megan Loring, MD, who specializes in minimally invasive gynecological surgery, has performed only three open procedures since joining the medical staff in 2015.
“The patient’s BMI and surgical history can make performing a laparoscopic hysterectomy technically difficult and may rule it out for some surgeons,” she explains. “The same is true when big fibroids are present, making the uterus itself very large.” She completed a fellowship and is comfortable performing the vast majority of hysterectomies laparoscopically — a far easier experience for patients.
“It is almost always done as outpatient surgery, patients experience minimal pain, and they are back to normal activities within two weeks,” she adds. Outpatient laparoscopic hysterectomies are associated with far fewer 30-day complications compared with inpatient open surgery, as was noted in a paper co-authored by Dr. Loring (Journal of the Society of Laparoendoscopic Surgeons, 2015).
Elbow fractures in children
They are not the typical sports injury, says John Cahoy, MD, PhD, a pediatric orthopedic surgeon, but supracondylar humerus fractures are common, especially in children age three to seven. The injury represents approximately 10 percent of all childhood fractures.
“They typically occur when a child falls on an outstretched arm from a height, with some impact,” he says. “Falling from the monkey bars is an example.” Symptoms are sometimes only a swollen elbow and inability to straighten the arm. More often, there is a clear deformity and severe pain.
“When patients are brought to the Emergency Department, I see them there, and many are admitted for surgical treatment,” he notes. “Sometimes pediatricians send their patients to my clinic. Most do not require surgery. If the bone is only slightly displaced, the child’s arm can be put in a cast for three weeks, and it will heal on its own.”
When the bones are significantly displaced, and surgery is indicated, Dr. Cahoy places smooth pins percutaneously — without an incision. They remain in place for three weeks and can be removed in the office. “Whether the child has surgery or not, the biggest concern is achieving full range of motion, which can usually be accomplished with simple stretches done with parents at home,” he adds.
Advanced surgery for bladder cancer
Orthotopic neo-bladder surgery is a reconstructive surgical option for bladder substitution available to patients with advanced bladder cancer.
“When surgical removal of the bladder is indicated, the number one question is ‘will I be left with a urinary bag?’ Today, the answer is no,” says Jason Gee, MD, urologist. “We can use the patient’s own intestines — the small or large bowel — to create a new bladder. It’s a specialized and important surgical procedure that provides patients with lower urinary tract function. We perform neo-bladder surgery at Emerson.”
Those who are unable to have orthotopic neo-bladder surgery are offered the continent catherizable pouch. “This is an internal reservoir that functions as a bladder with an opening at the skin surface,” says Dr. Gee. “The pouch is catheterized, but this avoids having the patient wear a urinary bag.
“The latest research is focused on identifying molecular markers to help us determine which patients will benefit from these approaches so that we can better select patients for organ-sparing treatment vs. bladder removal,” he adds.

